What is Coronary Heart Disease? Coronary Heart Disease tends to develop when cholesterol builds up on the artery walls, creating plaques. These plaques cause the arteries to narrow, reducing blood flow to the heart, or can cause inflammation in and hardening of the walls of the blood vessel. If you need assistance with writing your nursing literature review, our professional nursing literature review writing service is here to help!
What is Coronary Heart Disease?
INTRODUCTION
Heart disease is one of the leading causes of mortality in women across the world Rollini. In the United States, cardiovascular disease Carey, specifically coronary heart disease, is the leading cause of death among both men and women [nih coronary heart disease, Rollini]. Death from a cardiac-related event is more common than death from all forms of cancer combined.
However, even though more women than men die from coronary heart disease [Carey], heart disease itself is still commonly considered to be a male disease. Historically, medicine has utilized the man as the standard, even when treating women [xhyheri]. Therefore, there is the likelihood that it is under-diagnosed in women. This is because women suffer symptoms and respond to diagnostic testing differently than do men. Women also experience outcomes that are different than those men experience following intervention.
“Heart disease” is a term that is frequently used interchangeably with the term “cardiovascular disease”. Cardiovascular disease commonly refers to those conditions that involve blocked or narrowed blood vessels that can subsequently lead to heart attack, stroke, or angina. There are other heart conditions that can affect the heart’s muscle, beating rhythm, or valves, such as infections, that are also thought of as heart disease [mayoclinic]. Much of heart disease can be treated or prevented by making healthy lifestyle choices, such as a healthy diet, exercise, not smoking, and watching how much one drinks.
As of present, few studies specifically examine heart disease in women. Women in fact represent less that 30% of study population in the majority of clinical trials [Rollini]. The research that has been conducted has indicated that women are less likely to be diagnosed or treated as well as men [xhyheri]. Additionally, studies have indicated that women react differently to drugs typically prescribed to cardiovascular disease.
Additional research involving women, along with gender-specific analysis is needed. This would include the incorporation of more women into cardiac trials as well as into observational studies, and the usage of statistical techniques that enable testing for certain sex interactions and provide information about differences in response to treatment that are sex-specific.
Heart disease in women
Heart disease is the foremost cause of morbidity and mortality in women. However it is often under-recognized by both patients and providers, as women believe that the major killer – and therefore the disease they need to be on the lookout for – is cancer. Additionally, heart disease is still in large part considered a male disease, and the main emphasis in heart disease research and clinical practice has generally focused on men (Stranges).
However, a major shift has occurred recently, with greater recognition of the clinical significance of cardiovascular disease in women [1,5 in Stranges]. The realization of the importance of cardiovascular disease in women has also been accompanied by a growing awareness of differences in risk factors, treatment, preventative strategies, and prognosis of the disease [1, 5, 12-15 in Stranges] between the genders.
Some cardio-metabolic risk factors are either unique or more prominent in women than they are in men [5]. For instance, preeclampsia is lined to an increased risk of various cardiovascular outcomes later on in life [17]. Additionally such conditions as autoimmune diseases and depression can contribute in a disproportionate way to cardiovascular risk in women [5, stranges]. T
he prevalence of a number of traditional risk factors are also different for women than they are for men. For example, the prevalence of diabetes mellitus is greater among women in the U.S., primarily as a result of a decrease of level of physical activity as well as a difference in longevity between the genders [2, 5,18 in Stranges]. In fact, type 2 diabetes and impaired glucose tolerance are recognized as very strong risk factors for cardiovascular disease in women [19].
Additionally, type 2 diabetes and impaired glucose tolerance may increase the risk of recurrent cardiovascular events following the first acute myocardial infarction, particularly in women [20 stranges]. Hypertension also tends to be higher in older women, which contributes to the greater morbidity and mortality in women from stroke than in men [2, 21 Stranges]. Additionally, atrial fibrillation is a primary risk factor for ischemic stroke in women [5, 21], which has led to the development of management guidelines designed to prevent stroke in women [22].
Epidemiology
Heart disease is one of the leading causes of mortality across the world. In the United States, a woman dies from a heart related episode every minute [Rollini], and despite declining trends seen in many countries over the past 40 years in both men and women, cardiovascular disease is still the leading cause of mortality in both men and women [1-3 stranges]. Cardiovascular disease in fact is the cause of a greater number of deaths than all other chronic conditions combined, including cancer, neurodegenerative and respiratory diseases, and accidents [2].
Approximately 1 in every 3 women (34.9%) in the U.S. has some kind of cardiovascular disease. The percentage for men is slightly higher at 37.6% [zhang]. Approximately 1 in every 2.7 women will die of a cardiovascular disease; this is compared with approximately 1 out of every 4.6 women who will die of cancer [1 in zhang]
Although age-adjusted mortality rates of cardiovascular disease are higher in men than in women, the total number of cardiovascular disease related deaths has been consistently higher in women than in men for the past two decades, primarily due to a longer life expectancy as well as a larger proportion of elderly women [1,2 stranges]. Additionally, in the United States more hospitalizations occur for heart failure and stroke in women as compared to men [2]
Recent evidence indicates an increasing trend in coronary heart disease mortality in younger women. In U.S. women ages 35 – 44 years of age, coronary heart disease mortality rates have increased an average of 1.3% each year since 1997 [4]. These trends are most likely driven in part by the obesity and diabetes problem in the U.S., but other contributors include a decrease in physical activity and an increase in the prevalence of hypertension [4].
The escalation in prevalence of large scale cardiovascular disease risk factors in younger adults, primarily hypertension and obesity, as well as the leveling off or possible reversal of cardiovascular mortality trends is happening in the U.S. as well as in areas around the world, including the Mediterranean and Asia. These regions are classically associated with healthier dietary choices and lifestyles (6 -11 stranges]
Specific to the disease burden and the specific aspects of cardiovascular disease in women, the American Heart Association developed evidence-based guidelines specifically for women [12 – 15 stranges]. The most recent update of these guidelines was published in 2011 [12] and represented a major contribution to the field of cardiovascular disease management.
The focus of the guideline shifted from evidence based to effectiveness based, and considered both harms/costs and benefits of preventive intervention [12]. This shift indicates a major evolution from the guidelines revised in 2007, which were based mainly on the clinical benefits of intervention for cardiovascular disease prevention in women [15].
Additionally, the 2011 guidelines introduced “ideal cardiovascular health” as the lowest risk category, meaning that the presence of ideal levels of cardiovascular risk factors and adoption of a healthy lifestyle is most likely to be associated with favorable outcomes and a nicer quality of life, as well as increased longevity [50]. However, only a very small percentage of U.S. women will be classified as being at ideal cardiovascular health [51].
Differences in short term prognosis and clinical presentation between men and women are evident with cardiovascular disease. Especially in younger women, higher fatality rates have been seen during the 30 days first following an acute cardiovascular event, as compared with younger men [31, 32 stranges].
There has also been an ongoing debate on the reasons cardiovascular disease is managed differently in men and women [33-35], although there has been an improvement in the quality of care and in outcomes for women in recent years who have been hospitalized for cardiovascular disease [36 stranges]. There is some belief that gender disparities are the result of lower awareness of cardiovascular disease risk in women, as well as a delay in emergency services access. However, the gender gap has been reduced over time [37 stranges].
There is still work to be done, though, since very few clinical trials publish results that are sorted by sex. Additionally, researchers frequently utilize historical data in comparing clinical characteristics and treatment in both men and women, and many early trials had an upper cutoff age of 65 years, which excluded many women, since women develop cardiovascular disease on average ten years later than do men.
Also of concern is that the demographics of the U.S. – and in fact the world – are changing, which will mean that practitioners must consider a greater diversity of patients. Added to the well-known classifications of race and geographic origin as well as ethnic origin, there are other facets of diversity that must be considered. These include age, language, literacy, disability, socioeconomic status, religious affiliation, occupational status, and culture. Not only do these factors affect how cardiovascular disease presents and progresses, they also often affect the level of care the individual receives.
A report done by the Institute of medicine states that differences in treatment in women do exist even when controlling for such factors as comorbidities and insurance status [52 from mosca]. Pervasive disparities in the treatment of cardiovascular problems are a serious public health issue in the U.S. in spite of the marked declines in mortality that have been observed on a national scale over the past several decades.
These disparities in particular have an adverse impact on the clinical outcomes and quality of life for African American and Hispanic women, a fact which must be recognized by practitioners. Care that is sensitive to cultural difference includes the revision of healthcare delivery to meet the specific needs of a patient population that is incredibly diverse. Therefore diversity in this context of healthcare means that all individuals must receive equitable care, regardless of any barriers that may exist [57=59 mosca].
The main cause of these barriers to equitable care includes lack of understanding about patients’ health beliefs, cultural values, and frequently the inability to communicate symptoms accurately in what to many of these women is a foreign language [53-55 mosca]. General guidelines for diagnosis and treatment apply across all groups of women; however, it is important to note that risk factors such as hypertension are more prevalent in African American women. Also, diabetes mellitus is more prevalent in Hispanic women [6 from Mosca].
Most notably, the most coronary heart death rates and the greatest overall cardiovascular disease morbidity and mortality occur in African American women. This means that mortality from cardiovascular events in these women is more similar to those seen in men than those seen in other groupings of women. This simply underscores tat need for greater preventative efforts in some groupings of women as well as a different approach taken to diagnosis and treatment of cardiovascular disease, an approach more tailored to each specific grouping.
Deaths from cardiovascular disease have decreased in all groupings of women. However, Hispanics have the lowest percentage of deaths from cardiovascular events (21.7%) as compared with non-Hispanics (26.3%) [62 mosca]. Hispanics also have a longer life expectancy at 83.1 years compared with the 80.4 year life expectancy for non-Hispanic white women and the 76.2 years for non-Hispanic black women [63 mosca]. This means that cardiovascular complications due to age are a greater consideration for Hispanic women.
Age is not only a consideration for Hispanic women, however. The life continuum of women frequently reflects different events that are approached with different levels of stress – both physical and mental – than those that affect men. These events include such conditions as pregnancy. Therefore, it is important to consider all facets of diversity when practitioners care for women with cardiovascular disease, to avoid a disparity in care [64-66 mosca].
Etiology
Cardiovascular disease is largely caused by risk factors such as unhealthy lifestyle choices. Many of the causes for most forms of cardiovascular disease can be treated or prevented by making healthy lifestyle changes. These causes include:
Pathophysiology of heart disease
It is of utmost importance for the practitioner to recognize that women’s hearts are different from men’s hearts. While this area of study is somewhat new, it is known that women have smaller hearts as well as smaller arteries than men. Researchers from Columbia University and NY Presbyterian also believe that women have a different internal rhythmic to the pace of their hearts, which in general causes the heart of a woman to beat faster than the heart of a man. The researchers also believe that a woman’s heart may take longer to relax following each beat.
Additionally, some surgeons have hypothesized that the reason that women have a 50% higher chance of dying during heart surgery as compared to men may be related to a fundamental difference in the way a woman’s heart works. These differences may also be linked to the fact that women are more likely than are men to die after their first myocardial infarction [Ricciotti]. Approximately 25% of men die in the first year following their first myocardial infarctino, compared with 38% of women [Krupa online]. Women are also approximately twice as likely to experience a second myocardial infarction within 6 years of the first. Additionally, women are approximately twice as likely to die following bypass surgery. From Ricciotti online
Heart disease itself therefore affects the hearts of women in different ways than it does men. Following a heart attack, a woman’s heart is more likely to sustain its systolic function effectively. C. Noel Bairey Merz, the Director of the Women’s Heart Center at Cedars-Sinai Heart institute, has suggested that this reflects that cardiovascular disease affects the microvasculature in women, while in men it affects the microvasculature [Krupa].
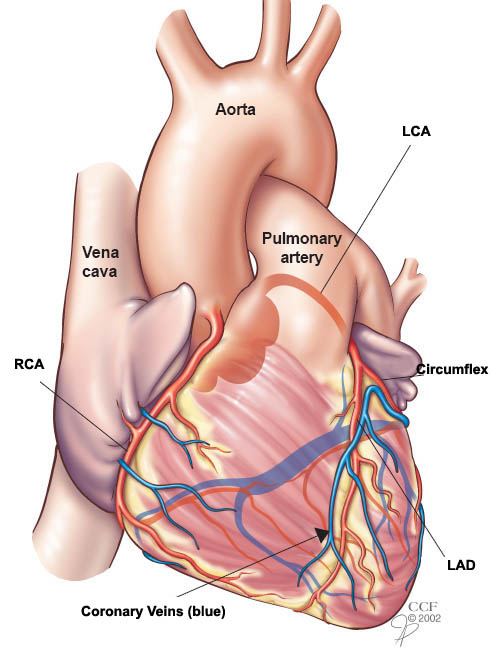
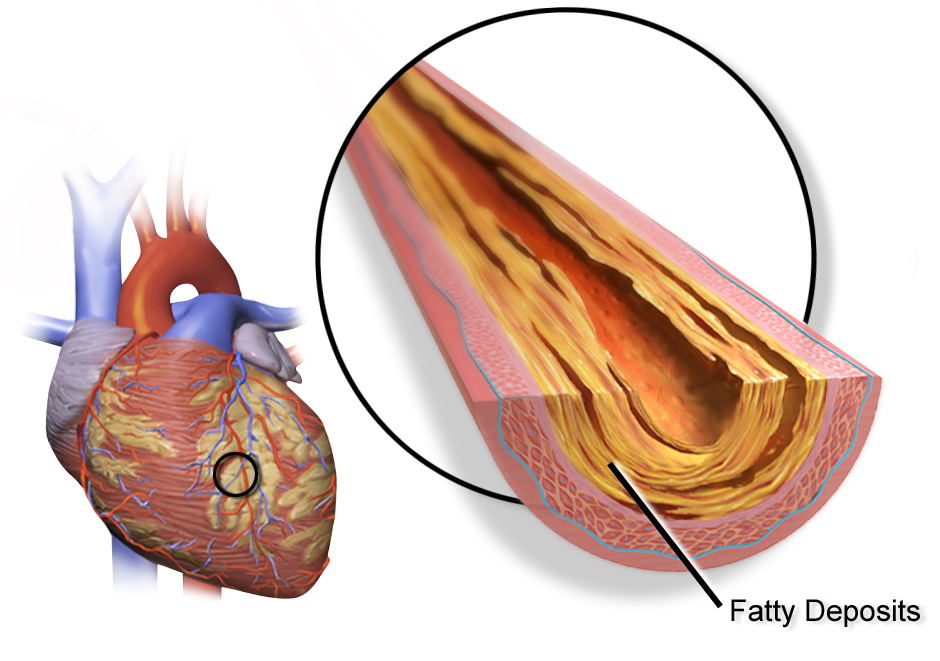
Conventional research has indicated that the most prevalent form of cardiovascular disease is coronary artery disease, where plaques narrow or block the major arteries of the heart, which in turn cuts off the supply of oxygen to the heart. The duration and severity of the impairment determines the severity of the acute event – unstable angina or myocardial infarction can result. This ultimately affects the heart’s ability to pump blood correctly. However, Bairey Merz found that women’s hearts were much less likely than were men’s to lose the ability to pump blood following a myocardial infarction.
Additionally, women were much less likely to present with coronary artery disease that was obstructive. This led Bairey Merz to conclude that in women the oxygen deprivation to the heart and the ensuing damage is more likely to happen when the small blood vessels become dysfunctional, as opposed to the major arteries [Krupa-online]. Bairey Merz further believes this is a major reason why women are misdiagnosed or suffer adverse heart events, beause practitioners typically look for the patterns of cardiovascular disease progression that are present in men as opposed to searching for patterns that are present in women.
The Women’s Ischemic Syndrome Evaluation (WISE) study concurred and has indicated that women may experience chest pain and abnormal stress testing even when there is no critical, flow limiting lesion (>50% luminal stenosis in a coronary artery) present in one of the major arteries. In this study, 60% of women who underwent coronary angiography did not have a lesion present. Even without experiencing critical blood flow problems, women in the study without lesions experienced persistent symptoms.
The persistence of the symptoms, combined with abnormal stress testing results was therefore attributed to endothelial dysfunction and disease affecting the microvasculature. A number of factors may contribute to endothelial dysfunction and disease affecting the microvasculature. Hypertension, LDL cholesterol, diabetes, the chemicals in tobacco, circulating vasoactive amines, and infections can all contribute.
Women are not beyond danger regarding plaque and disruption of forward blood flow in the arteries, however. This is primarily because women have smaller coronary arteries than do men, even after correcting for total body surface area [7 Kusnoor]. Therefore, anything that affects flow may prove to be critical. Additionally, women are two times more likely than men to have plaque erosion with subsequent blood clot formation [8 kusnoor]. From Kusnoor online bookmarked
Risk Factors
From Schenk-Gustaffsen
Risk factors for heart disease are roughly the same for both sexes; however, gender specific differences are present (Rollini). There are some unique risk factors that exist for women; older age at presentation is a major risk factor, as women are more likely to suffer from comorbities, including diabetes and hypertension.
Given the fact that 6 out of every 10 deaths [schenk] from cardiovascular disease in women can be prevented, it is extremely important to understand the risk factors associated with the disease in women.
According to the Inter Heart study [2 schenck] there are nine factors that are responsible for 90% of all cardiovascular disease cases. These factors are:
Smoking
Stress
Dyslipidemia
Diabetes
Hypertension
Obesity
Poor diet, particularly one that does not include sufficient intake of fruits and vegetables
Physical inactivity
Consumption of alcohol in excess
The same cardiovascular risk factors have been used in risk calculations for the past 40 years, despite increasing knowledge regarding gender differences and the disease. Ridker et al [schenck, find ref] suggested in 2007 to use the Reynolds scoring system for women. This suggestion is based on a 10 year study of data from the Women’s Health Study for cardiovascular events in 25,558 women, all over 45 years of age. The conclusion was that this scoring system predicted cardiovascular disease risk in women better than classical scoring systems.
Modifiable
Diabetes mellitus is one of the most important risk factors, and coronary heart disease mortality is 3 – 5 times higher in those women who are diabetic as compared to those who are not diabetic. In contrast, the risk is only 2 – 3 times higher in men who are diabetic. Women also have a 3 – 5 times higher chance than men of developing cardiovascular disease to begin with [30 schenck]. Higher glucose levels as well as insulin resistance serve to counter the protective effects of estrogen, which places women at this higher risk [Johnson].
Cardiovascular events are the primary cause of death, particularly in type II diabetes. The Nurse’s Health Study indicated that coronary heart disease mortality in women who have diabetes was 8.7 times higher than non-diabetics [31 schenck]. An additional danger is that women who are diabetic develop cardiovascular disease earlier, at approximately the same age men do. Why this is the case is currently unknown [33]. Diabetes is largely preventable or well-controlled through making healthy dietary and fitness decisions, sometimes in tandem with medication.
Cigarette smoking is a very significant risk factors for coronary heart disease in women. Smoking in women prompts more negative cardiovascular and lung consequences than does smoking in men. One potential reason for this may be that the dimensions of the coronary arteries and the lungs are smaller in women than in men; therefore, a woman smoking the same amount as a man would do more damage to her body.
Women who are less than 55 years of age have 7 times increase in risk attributable to smoking than do men, and the increase in risk depends on dose. It is undisputed that smoking predisposes the individual to atherosclerosis [24, 25 schenck]. The Nurse’s Health Study, which examined more than 120,000 healthy nurses, indicated that only 4 – 5 cigarettes a day nearly doubled the risk, and 20 cigarettes a day compounded the risk 6 times [26 schenck].
Smoking has declined a bit in men; however smoking in women has not declined at the same rate, particularly in younger women. This can lead to significant vascular problems later on in life. Further, individuals who are routinely exposed to second hand smoke see a 25% increase in the risk of developing cardiovascular disease.
Therefore, it is not simply direct smoking that causes the problem. Additionally, smoking combined with other factors – such as use of contraceptives containing estrogen – multiplies risk for cardiovascular events and for clot formation [ROllini]. Hormonal contraception is in fact contraindicated for women over 35 years of age who smoke as a result of the multiplied risk. Refraining from smoking lessens the risk of developing heart disease and helps reduce potential cardiovascular risk factors.
Alcohol consumption poses a risk for the development of cardiovascular disease. A moderate intake may be protective to the heart, but too much alcohol is harmful [45, 46 schenck]. The type of alcohol consumed is not as crucial as are the drinking patterns. Low to moderate daily intake may be protective, whereas conversely binge drinking can be harmful to the heart. If a patient has already experienced a first myocardial infarction, it is not necessarily a bad thing to continue drinking moderately.
However, it is also not necessarily recommended that patients start drinking in search of the protective benefits of alcohol consumption following a first myocardial infarction [schenck]. Light to moderate drinking is defined as defined as one standard drink for women per day and two per day for men. The difference exists because men and women metabolize alcohol differently; specifically women metabolize slower than do men. A standard drink is defined as 12 grams of alcohol; this is equivalent to 15 cl of wine.
It is well established that there is an association between LDL cholesterol and an increased risk of cardiovascular disease. Individuals who reduce their LDL cholesterol also reduce their risk for cardiovascular disease. Further, this reduction in combination with raising their HDL cholesterol serves to further reduce risk. A study conducted by the Lipid Research Clinic indicated that low HDL cholesterol in women was the most significant predictor of death from ischemic heart disease [12 schenck]. It has been shown that having low HDL levels affects women more than it does men [16 schenck], so it is important that practitioners encourage the reversal of low HDL.
Hypertension is also a risk factor for cardiovascular disease. A meta-analysis that included data from more than 1 million adults ages 40 – 69 indicated that an increase of 20 mmHg systolic or 10 mmHg diastolic in an individual’s normal blood pressure doubles the mortality from coronary heart disease [22 schenck]. There is a 3 times increase in coronary heart disease as well as stroke in women with >185 mmHg systolic when compared to women who are less than 135 mmHg systolic [23 schenck]. The way hypertension is treated is currently the same in both emn and women. Most of the time, pharmacotherapy and lifestyle changes is the preferred treatment.
A sedentary lifestyle and obesity pose a significant risk as well. Obesity is more common in women (35.5% ) than in men (32.2%), and 27% of women are obese [1 schenck]. People who are active and regularly exercise their heart muscle are at a much lower risk of developing heart disease. In particular, obese women are more likely to also have metabolic conditions such as polycystic ovarian syndrome or Syndrome X than are lean women, which multiplies risk [Johnson].
Exercise and physical fitness play a big role, and lack of physical activity is a major risk factor for developing cardiovascular disease. One study found that less fit individuals experiences a 4.7 times increased risk of stroke and myocardial infarction, independent of other risk factors [37 schenck]. The beneficial effects of exercise are not as great in women as they are in men; women experience smaller increases in HDL resulting from similar exercises as men [38 schenck].
The Nurses’ Health Study has indicated though, that two aspects are particularly beneficial to women, namely that brisk walking delivered the same benefits as did vigorous exercise, and women who had previously been sedentary experienced benefits that were similar to those who had exercised earlier in life. This means that it is better to exercise late than to never do so. The recommended amount of exercise is 30 minutes of exercise daily.
Diet. A poor diet is a major risk factor for the development of cardiovascular disease. The Mediterranean diet has been shown to have beneficial effects on alleviating cardiovascular disease risk. The diet has a high proportion of fruits and vegetables, and has a positive impact on total cholesterol, LDL cholesterol, blood pressure, and myocardial infarction [47 schenck].
One study of 600 men and women who were randomized into either a group using the Mediterranean diet or a control group indicated that after 27 months a marked difference was found in mortality and morbidity for cardiovascular disease as well as total mortality in favor of the Mediterranean diet [48 schenck]. The mechanisms behind this are multiple, with the recommendation that diet always be combined with other changes to lifestyle, such as exercise or medication. The effects are likely the same in women as in men, but there has not been much gender specific research into why the Mediterranean diet proves beneficial [49, 50 schenck]
Depression serves as a risk factor for the development of cardiovascular disease, particularly if the patient is also taking antidepressant medication. Mood in general is a risk factor, particularly if the individual experiences a high level of stress on a consistent basis. As compared to other risk factors, psychosocial variables are much more difficult to define or to measure objectively. Nonetheless, there are several different aspects within the broad definition of psycho-social factors that are currently associated with increased risk of myocardial infarction.
These aspects include work and family stress, lack of control, low socioeconomic status, negative life events, and a poor social support system. These aspects, along with depression, affect the risk of ischemic heart disease as well as the prognosis. There are several studies that show a clear correlation between stress and cardiovascular disease. One study indicated that family stress – including marital stress – increases the risk of ischemic heart disease [41 schenck].
Another study indicated that work stresses as well as home stresses were more common in those patients who had suffered a myocardial infarction, and that stress represented 30% of the individual’s total risk [42 schenck]. Where depression is involved, it has been found that both women and men tend to get more depressed following myocardial infarction [43, 44 schenck]. This increases the risk of a second myocardial infarction. It is important to note regarding depression that more women experience depression than men, and it is therefore a more important risk factor in women.
Recent evidence indicates that sleep deprivation and disturbances may be associated with cardiovascular disease, particularly in women [23 stranges]. Three independent studies have indicated an association between increased hypertension and sleep deprivation. This phenomenom occurred only in women [24 – 26 stranges]. These findings are particularly significant because sleep disturbances and deprivation are more common in women than in men in both developed as well as developing countries [27, 28 stranges]
Non-modifiable
Genetics. Congenital heart disease is something the individual is born with. However, an individual may also have a genetic predisposition to develop certain cardiovascular problems, as seen through examining family history of heart disease. In the latter, a predisposition does not mean the individual is guaranteed to develop the specific cardiovascular problem they are predisposed to; healthy lifestyle choices such as eating well, not using alcohol to excess, not smoking, and exercising regularly can go a long way toward fighting genetic predisposition.
It is interesting to note that simply having a family history of the disease can lead to stress and disruption in mood for some individuals, both risk factors for cardiovascular disease. In one study that examined data collected from 60 women and 31 men who averaged 21.4 years of age it was found that a family history impacts stress responsiveness, which can contribute to future heightened cardiovascular disease risk [wright].
Menopause poses a risk for coronary heart disease in women because the reduced production of estrogen leads to worsening of coagulation, vasculature, and the lipid profile. Early menopause in particular is a known risk factor; results of a study utilizing the Women’s Ischemic Syndrome Evaluation (WISE) indicate that estrogen deficiency poses a very strong risk factor for coronary heart disease
Read More On
- What is combined pulmonary fibrosis and emphysema?
- Why is reflection important in mental health nursing?
- Evidence Based Practice requirements that all healthcare professionals need to understand.
- HIV/AIDS effects in the population and the factors contributing to its spread
- Why is Brazilian But Lift a dangerous cosmetic surgery.
Do not hesitate to contact our professionals if you need help with your essay even after going through our example guide.


